UW Ophthalmologist will help design a sensor that monitors biomarkers
Yes, eyes are the windows to your soul. But your tears, it turns out, have their own story to tell.
"We tear all the time, not just when we cry, and our tears are actually very similar to blood," said Tueng Shen, MD, PhD, Professor of Ophthalmology, Graham and Brenda Siddall Endowed Chair and Associate Dean: Medical Technology Innovation (UW School oif Medicine/College of Engineering).
“Just like saliva and sweat, tear film carries biomarkers — proteins, molecules and other substances that indicate what is happening inside the body.”
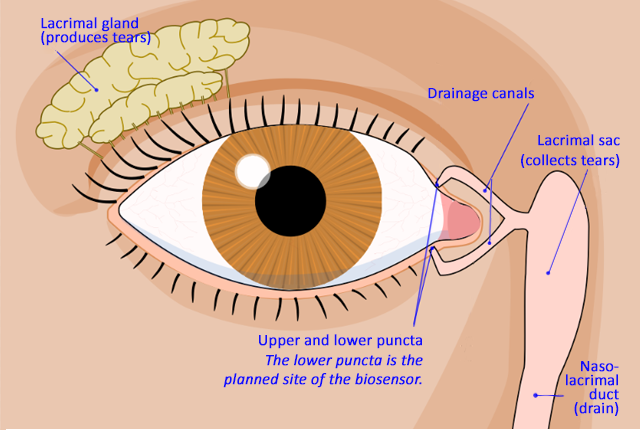
Shen is guiding the design of a microscopic wireless biosensor that would sit in a tear duct, a space roughly 1 to 2 millimeters across, and continuously monitor the fluid for signs of disease.
The idea is funded through ARPA-H, the Advanced Research Projects Agency for Health, a federal office focused on health innovation.
In the project’s proof-of-concept phase, the sensor would focus on two targets: inflammation and blood-sugar levels.
Inflammation, measured through a molecule called IL-6, is relevant to a range of conditions, including dry eye disease. Glucose levels in tears correspond to blood-sugar levels in the body, Shen said, suggesting that the device might be a non-invasive way to track whether a chronic condition like diabetes is well-managed.
"We could sample the tear components minute by minute, pretty much continuously," Shen explained." That stands in contrast to blood draws, which capture the body’s information only in a single moment.
The teeny, implanted sensor would be programmed to identify specific proteins or molecules. It would need to detect, power and wirelessly transmit health data for an ARPA-H directed span of at least six months. The team is exploring whether the sensor could harvest energy from the body itself.
It’s a lot of capability to build into something the size of a grain of rice.
The idea “pushes our engineering limits,” Shen acknowledged. “But I’m excited because if we can do this in a space as small as a tear duct (puncta), we can use the same technology in a much bigger space like the skin or the intestine. I see this as a broad health-monitoring platform if we can make this test work.”
The device would be manufactured using 3D-printing techniques developed by Northwestern University, one of three partner institutions on the project, alongside UW and the Massachusetts Institute of Technology.
The design is modeled on a plug commonly placed in the eye's lower puncta, or tear drain, as a therapy for dry eye. Because those plugs are well tolerated by patients and can remain in place for roughly six months, the research team is targeting the same lifespan for the biosensor. The insertion procedure would require no surgery and minimal anesthesia.
Shen’s role is to give clinical parameters on the device’s sensors, including obtaining a chemistry of tears to establish the range of concentration for biomarkers.
UW's participation represents a program that meshes engineering more directly with medicine, formally called KEMi (Kren Engineering-based Medicine Initiative).
The broader ARPA-H initiative (ARPA-H-SOL-25-115) supporting this work is called OCULAB.